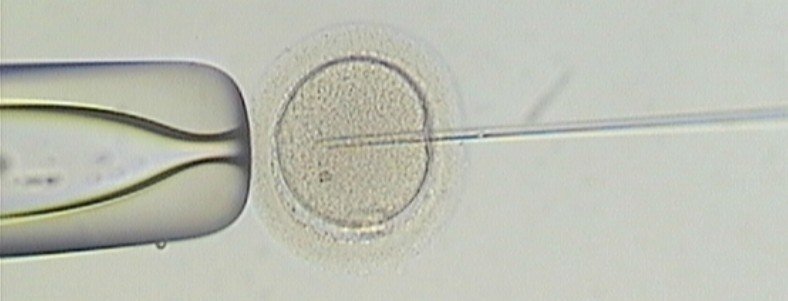
Intracytoplasmic Sperm Injection
ICSI (intracytoplasmic sperm injection) is a procedure whereby a single sperm cell is injected into an egg cell. In natural conditions, the sperm would use chemicals located in the head to bore through the egg’s “shell”. It is technically an IVF procedure as it is performed ‘in vitro’ (literally means ‘in glass’, contextually it means ‘within a test tube’). As you may have gathered, ICSI should mostly be used in cases where it is the male who is subfertile. The procedure of injecting a sperm into an egg bypasses the natural process.
This procedure was perfected quite recently, with the first human pregnancy generated by ICSI being in 1991. It brought with it a revolution in the IVF world due to the fact that it required only 1 sperm per egg. If we compare this to the natural process once more, we may remember from school that hundreds of millions of sperm compete with each other to reach the egg. ICSI bypasses this completely and allows subfertile men to achieve similar pregnancy success rates to other men having IVF
This breakthrough of a procedure has a simple caveat, however. What happens to the children born through ICSI? Well, they seem to be mostly without any major issues except possibly when it comes to fertility. It seems that ICSI could be contributing to low male fertility in the very children born through the procedure. F Belva et al published a study in 2016 in ESHRE describing these results. “Our findings are robust even after adjusting for covariates that are generally known to affect sperm parameters. In our data, no correlation between BMI, season of sampling, smoking alcohol consumption and drug use could be found with any of the semen parameters.”
A link between ICSI and low fertility in sons
The sample of the 54 men, now aged 18-22 and born after their fathers used ICSI, all seemed to have low sperm concentration, low sperm count and even low total motile sperm count. So what is it about ICSI that causes this reduction in male fertility? Unfortunately it’s very hard to determine. The team were even unable to determine if there was a direct fertility correlation between fathers and ICSI sons.
Are these results reliable?
The sample size of 54 is too small to give unarguable results, another sample may result in the opposite. Nevertheless, the dramatic findings of the study demand further investigation. Other studies have suggested that there is no causal relationship between the ICSI process and reduced male fertility. They suggest instead that the observable small decline in the fertility of male children born through ICSI is because of the underlying genetic condition of the father being passed to the offspring, and without ICSI the father simply wouldn’t have children. And whilst considering this whole subject one has to take into account the results of other, major, studies which appear to show a huge decline in general male fertility around the world over the last few decades. Thus male-factor infertility still remains a mystery in terms of its origin. The missing link is still out there. For now, the miracle of ICSI is met with this trade off. Hopefully with due time, the enigmatic origins of male infertility will be unravelled.
Widespread use of ICSI
Until the causes of male infertility are known better, what should we do about it? Here at Concept Fertility we usually say simplest is best and we only recommend ICSI when we believe it is necessary. This is the same for all other elements additional to basic IVF. We find that we end up using ICSI in less than a third of our IVF cases. More widespread data is difficult to find but it seems to be policy in some clinics, and some countries, to use ICSI in 100% of IVF cycles. We believe this increases fertilisation rates but not viability rates. In other words, more eggs become embryos one day later but a few days after that the percentages surviving are very similar. We believe our own ongoing pregnancy rates are good and do not suffer as a result of our low use of ICSI. So, even though we believe there may be no underlying risks from ICSI, why take the risk of using an additional, unnecessary procedure?